Erythema Multiforme
July 8, 2025 | Black & Kletz Allergy
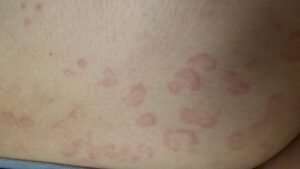 Erythema Multiforme is a type of a rash on the skin, usually triggered by an infection or an adverse effect of a medication. The condition gets its name from the appearance of reddish skin lesions of various forms seen at the same time.
Erythema multiforme affects less than 1% of the population. It is most common in young adults (aged 20 - 40 years) with a modest predominance in males. Some people are genetically predisposed to develop erythema multiforme.
Causes:
Erythema Multiforme is a type of a rash on the skin, usually triggered by an infection or an adverse effect of a medication. The condition gets its name from the appearance of reddish skin lesions of various forms seen at the same time.
Erythema multiforme affects less than 1% of the population. It is most common in young adults (aged 20 - 40 years) with a modest predominance in males. Some people are genetically predisposed to develop erythema multiforme.
Causes:
Erythema multiforme is an immunological response to either an infection or a medication, manifested on the skin. The most common causative factors are:
- Infections - Herpes simplex virus (most common), mycoplasma, cytomegalovirus, Epstein-Barr virus, influenza virus, coronavirus, etc.
- Medications - Antibiotics (e.g., sulfonamides, tetracyclines, erythromycin), aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs) (e.g., ibuprofen, naproxen), anti-seizure medications, and vaccines.
- Systemic disorders - Inflammatory bowel disease, hepatitis, lymphoma, leukemia, and solid organ tumors.
- After exposure to the trigger, there is usually a prodromal period when the individual may experience mild fever, cold like symptoms, sore throat, headache, fatigue, and/or achiness.
- A few days later, the typical skin lesions will erupt. These lesions may be in the form of red papules (i.e., small raised bumps), vesicles (i.e., blisters filled with clear fluid), ulcers (i.e., skin sores), etc.
- Characteristic lesions are ‘bulls-eye’ target lesions with a central dusky area, surrounded by a pale edematous area and a peripheral reddish ring, demarcating it from the surrounding normal skin.
- Atypical lesions are raised with poorly defined borders and/or fewer zones of color variation.
- Several lesions in different developmental stages may be seen at the same time.
- The skin lesions are usually symmetrical, begin at the periphery and spread centrally. The skin lesions usually have a predilection to extensor surfaces (i.e., outer side of the limbs)
- Skin lesions may be very itchy, painful, and/or swollen.
- Confirmation of the diagnosis may require a skin biopsy.
- Tests for infections, especially herpes simplex virus, are needed.
There are 2 types of erythema multiforme:
- Erythema multiforme minor - Mild form of the illness that only affects the skin and causes a rash.
- Erythema multiforme major - Most severe form of the condition which may be life-threatening because it causes large areas of the skin to blister and peel. This type affects the mucus membranes in the mouth, eyes, and genitals. Individuals usually have systemic symptoms such as fevers and/or joint pain.
- Most cases of erythema multiforme are mild and self-limiting and usually resolve spontaneously after a few days or weeks.
- Antihistamines and topical corticosteroid medications are helpful in relieving the itching and discomfort associated with more severe skin lesions.
- Antiseptic and local anesthetic mouthwashes may help relieve the pain and irritation associated with mucus membrane lesions inside the mouth.
- Antihistamine or anti-inflammatory eye drops can treat redness, burning, and/or excessive tearing of the eyes.
- Proper care of skin lesions such as avoidance of scratching will help prevent the spread of infections.
- Most severe cases may need a course of systemic corticosteroids such as oral prednisone.
- Recurrent cases are usually treated with 6 months or more of continuous oral antiviral medications such as acyclovir.
- General hand and respiratory hygiene is important in order to reduce the risk of contracting viral and bacterial infections.
- Avoiding medications that had previously caused adverse reactions in the past.
The board certified allergy specialists at Black & Kletz Allergy have 3 locations in the Washington, Northern Virginia, and Maryland metropolitan area. Our offices are located in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All of our offices have on-site parking and the Washington, DC and McLean, VA offices are also Metro accessible. The McLean office has a complementary shuttle that runs between our office and the Spring Hill metro station on the silver line. The allergists at Black & Kletz Allergy diagnose and treat both pediatric and adult patients. To make an appointment, please call our office or you may click Request an Appointment and we will respond within 24 hours by the next business day. The allergy doctors at Black & Kletz Allergy have been helping patients with allergic skin rashes, hives (i.e., urticaria), eczema (i.e., atopic dermatitis), as well as other causes of allergies including hay fever (i.e., allergic rhinitis), asthma, sinus disease, food allergies, medication allergies, insect sting allergies, and immunological disorders for more than 50 years. If you suffer from an allergic skin rash or any other type of allergies it is our mission to improve your quality of life by minimizing or preventing your unwanted and annoying allergy symptoms.
Prurigo Nodularis
June 27, 2025 | Black & Kletz Allergy
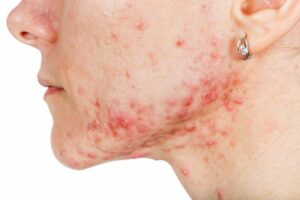 Prurigo nodularis is a chronic inflammatory skin disease where an extremely itchy rash in the form of firm bumps called nodules appears most commonly on the arms, legs, upper back, and/or abdomen. The rash is usually symmetrically distributed on both sides of the body. The itchiness, burning, and stinging sensation associated with prurigo nodularis is so severe that it often interferes with sleep and one’s psychological well-being.
The exact cause of prurigo nodularis is unknown, but altered function of the immune system and nerves in the skin is believed to be associated with heightened sensations of itchiness (i.e., pruritus) that leads to frequent scratching. Frequent scratching and picking of the skin are also thought to contribute to further lesion formation and thickening seen in the disease.
Prurigo nodularis can occur at any age but is more common in the elderly. When it occurs in younger patients, it is more likely to be associated with inflammatory skin diseases, usually eczema (i.e., atopic dermatitis). Prurogo nodularis is also more likely to manifest in patients with other underlying medical conditions that affect multiple body systems, such as cancer, diabetes, chronic kidney disease, and HIV infection. Prurigo nodularis is not hereditary or contagious.
The rash and itching can be episodic or continuous, lasting for several months in some individuals. It is typically worsened by sweat, heat, synthetic clothing, and/or stress. The rash can range in severity from just a few to several hundred lesions. The lesions can range in size from 0.2 inches to 0.8 inches wide and can appear as firm, dome-shaped papules, nodules, or plaques. Lesions can be flesh-colored, pink, red, brown, or black in color.
Diagnosis:
Prurigo nodularis is a chronic inflammatory skin disease where an extremely itchy rash in the form of firm bumps called nodules appears most commonly on the arms, legs, upper back, and/or abdomen. The rash is usually symmetrically distributed on both sides of the body. The itchiness, burning, and stinging sensation associated with prurigo nodularis is so severe that it often interferes with sleep and one’s psychological well-being.
The exact cause of prurigo nodularis is unknown, but altered function of the immune system and nerves in the skin is believed to be associated with heightened sensations of itchiness (i.e., pruritus) that leads to frequent scratching. Frequent scratching and picking of the skin are also thought to contribute to further lesion formation and thickening seen in the disease.
Prurigo nodularis can occur at any age but is more common in the elderly. When it occurs in younger patients, it is more likely to be associated with inflammatory skin diseases, usually eczema (i.e., atopic dermatitis). Prurogo nodularis is also more likely to manifest in patients with other underlying medical conditions that affect multiple body systems, such as cancer, diabetes, chronic kidney disease, and HIV infection. Prurigo nodularis is not hereditary or contagious.
The rash and itching can be episodic or continuous, lasting for several months in some individuals. It is typically worsened by sweat, heat, synthetic clothing, and/or stress. The rash can range in severity from just a few to several hundred lesions. The lesions can range in size from 0.2 inches to 0.8 inches wide and can appear as firm, dome-shaped papules, nodules, or plaques. Lesions can be flesh-colored, pink, red, brown, or black in color.
Diagnosis:
- The characteristic appearance and distribution of the lesions, the chronicity, and association with other systemic disorders provide clues to the diagnosis of prurigo nodularis.
- The confirmation of the diagnosis is established by biopsy of the skin lesions and examination of them under a microscope. It usually reveals thickening of different areas of the outermost layer of the skin (i.e., epidermis) with distinct changes (i.e., hyperkeratosis) to the skin protein keratin. The layer below the epidermis, referred to as the dermis, shows an increase in several inflammatory white blood cell types.
- Blood tests including a complete blood cell count (CBC), a comprehensive metabolic panel (CMP) that includes liver and kidney function tests, and a thyroid hormone panel may be beneficial for diagnosing an underlying systemic disease that may be contributing to the prurigo nodularis.
Treatment:
- Behavioral treatments for prurigo nodularis include ways to prevent scratching and dryness, such as keeping fingernails short, wearing long sleeves, wearing gloves, bandaging lesions, cleaning skin with gentle cleansers, keeping skin moisturized with non-irritating lotions, and avoiding warm environments to reduce sweating. Recommended anti-itch lotions include calamine, menthol, and camphor lotions.
- Moisturizers such as petroleum jelly, fragrance-free and ceramide-rich creams or ointments, and fragrance-free oatmeal or hyaluronic acid creams.
- Second generation oral antihistamines such as Zyrtec, Xyzal, Allegra, Claritin, or Clarinex taken on a regular basis. Many patients need 2 to 3 times the regular daily dose to get adequate relief from the severe itching and/or burning sensation that can be present in some individuals.
- Some patients respond better to first generation sedating antihistamines such as Palgic, Periactin, Atarax, or Benadryl.
- Topical medications such as corticosteroids (e.g., triamcinolone, fluocinonide, betamethasone, mometasone, clobetasol, fluticasone, desoxymetasone), calcineurin inhibitors (e.g., pimecrolimus, tacrolimus), capsaicin (the spicy ingredient in chili peppers), and vitamin D.
- Phototherapy: Exposing affected areas of the skin to specific wavelengths of ultraviolet (UV) light may help reduce the itchiness and inflammation of the skin.
- In 2022, dupilumab (i.e., Dupixent), an interleukin-4 receptor alpha antagonist, was approved by the U.S. Food and Drug Administration (FDA) to treat adults with prurigo nodularis. It is a subcutaneous (SQ) injection which can be self-administered under the skin every 2 weeks.
- In 2024, nemolizumab (i.e., Nemluvio), an interleukin-31 receptor antagonist, was approved by the FDA to treat adults with prurigo nodularis. It is a subcutaneous (SQ) injection administered every 4 weeks.
- Immunosuppressants such as cyclosporin, azathioprine, and methotrexate are reserved for the most resistant cases of prurigo nodularis because they affect more body systems and can have more serious side effects.
The board certified allergy specialists at Black & Kletz Allergy will promptly answer any questions you may have regarding prurigo nodularis or any other itching disorder. Our allergists have been diagnosing prurigo nodularis and other skin conditions in the Washington, DC, Northern Virginia, and Maryland metropolitan area for more than 50 years. We have 3 convenient locations in the DC metro area with offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. There is on-site parking at each location and both the Washington, DC and McLean, VA offices are Metro accessible. There is a free shuttle that runs between our McLean, VA office and the Spring Hill metro station on the silver line. To schedule an appointment, please call us at any one of our 3 locations. Alternatively, you can click Request an Appointment and we will respond within 24 hours by the next business day. Black & Kletz Allergy is dedicated in providing the most up-to-date diagnostic and treatment modalities in the field of allergy, asthma, and immunology.
Summer Outdoor Allergies
June 16, 2025 | Black & Kletz Allergy
 Now that Summer is almost here, people tend to spend a lot of time outdoors. Whether it be going to the beach, swimming at the neighborhood pool, playing baseball or softball, having a picnic, fishing, hiking, riding bicycles, gardening, or any other outside activity, people are more likely to be outdoors now than in any other season of the year. Since the general public is outdoors more in the Summers, it should be noted that there are a lot of outdoor allergens that they are being exposed to when outside.
The most obvious allergens that come to mind are the pollens, which are associated with late Spring and Summer. In the Washington, DC, Northern Virginia, and Maryland metropolitan area, tree, grass, and ragweed pollens make up the bulk of the pollens that tend to cause allergy symptoms in susceptible individuals. Tree pollen generally is released at the end of February and it lasts until late May or early June. Grass pollen, on the other hand, usually begins to pollinate in late April or early May and lasts until the end of August. Ragweed, a type of weed that is quite bothersome to some individuals, generally begins to pollinate in mid-August and ends after the first frost which is usually in late October.
The classic symptoms associated with pollen allergies typically include one or more of the following symptoms: sneezing, runny nose, nasal congestion, post-nasal drip, itchy nose, itchy mouth, itchy eyes, watery eyes, redness of the eyes, snoring, headaches, and/or sinus congestion. In those individuals with asthma whose asthma is exacerbated by pollen, chest tightness, wheezing, coughing, and/or shortness of breath may also ensue.
In addition to pollens as a source for summertime allergies, one must be cautious of flying insects, particularly if that person has a history of hives or a systemic allergic reaction resulting from an insect sting. In the Washington, DC metro area, bees, wasps, yellow jackets, white-faced hornets, and yellow-faced hornets are the major flying insects that inject venom into humans. Some individuals will naturally develop an immune response to further stings with that species of insect. As a result, when that person is subsequently stung with the insect that they are allergic to, an allergic reaction occurs which may be mild, moderate, or severe. Severe allergic reactions to flying insects due to venom allergy may be life-threatening. Anyone who has a history of hives and/or a systemic reaction to a flying insect, whether it be mild, moderate, or severe, should seek a board certified allergist to get evaluated. Allergy blood testing or allergy skin testing is warranted and depending on the results of the tests, a course of venom immunotherapy (i.e., allergy shots to venomous flying insects such as bees, wasps, yellow jackets, white-faced hornets, yellow-faced hornets) may be necessary as it is very efficacious in preventing further severe allergic reactions to flying insects if stung again. In addition, a self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine spray (e.g., Neffy) should be prescribed to anyone with a history of venom sensitivity and told to go to the closest emergency room if the epinephrine is used.
Another allergen lurking in the summertime is poison ivy. Together with poison oak and poison sumac, these plants are notorious for causing severe itching and rashes to sensitive individuals. In addition to the person who enjoys doing various activities outside, certain “outdoor” professions (e.g., construction workers, firefighters, farmers, landscapers) are at a higher risk to develop poison ivy, poison oak, poison sumac, or other plant-induced contact dermatitis than other professions where workers are primarily based indoors.
Certain groups of people or individuals are more prone to developing an allergy to sunscreen. Individuals who work outdoors on a regular basis such as farmers or construction workers, people with sun-damaged skin, and persons applying sunscreen to areas of damaged skin are more at risk. Females are more affected primarily because they are more prone to using cosmetics that can contain potentially irritating substances.
One should also remember that food allergies are always a problem, but may be a bigger problem if one is outdoors in a remote location far from an urgent care center or hospital. Thus, campers, hikers, and nature lovers should be very in tune to what foods they consume and avoiding those foods they are not supposed to eat. They should also carry their self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine spray (e.g., Neffy).
Black & Kletz Allergy has board certified allergy and immunology physicians as well as a trained staff experienced in both the diagnosis and treatment of atopic diseases such as allergic rhinitis (i.e., hay fever), allergic conjunctivitis (i.e., eye allergies), asthma, contact dermatitis (e.g., poison ivy, poison oak, poison sumac, sunscreen allergy), and food allergies. We treat both adults and children and we have 3 convenient office locations in the Washington, DC, Northern Virginia, and Maryland metropolitan area. Black & Kletz Allergy has offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. We have on-site parking at each location and the Washington, DC and McLean offices are Metro accessible. There is a free shuttle that runs between the McLean, VA office and the Spring Hill metro station on the silver line. Please call us if you, a family member, a friend, or a colleague suffer from any one of these maladies or any other allergic or immunologic problem and want to be evaluated and treated. You may also click Request an Appointment and we will respond within 24 hours of the next business day. The allergy doctors at Black & Kletz Allergy strive to keep up with the newest allergy and asthma treatment modalities so that cutting edge medicine is always at the forefront and available to our patients.
Now that Summer is almost here, people tend to spend a lot of time outdoors. Whether it be going to the beach, swimming at the neighborhood pool, playing baseball or softball, having a picnic, fishing, hiking, riding bicycles, gardening, or any other outside activity, people are more likely to be outdoors now than in any other season of the year. Since the general public is outdoors more in the Summers, it should be noted that there are a lot of outdoor allergens that they are being exposed to when outside.
The most obvious allergens that come to mind are the pollens, which are associated with late Spring and Summer. In the Washington, DC, Northern Virginia, and Maryland metropolitan area, tree, grass, and ragweed pollens make up the bulk of the pollens that tend to cause allergy symptoms in susceptible individuals. Tree pollen generally is released at the end of February and it lasts until late May or early June. Grass pollen, on the other hand, usually begins to pollinate in late April or early May and lasts until the end of August. Ragweed, a type of weed that is quite bothersome to some individuals, generally begins to pollinate in mid-August and ends after the first frost which is usually in late October.
The classic symptoms associated with pollen allergies typically include one or more of the following symptoms: sneezing, runny nose, nasal congestion, post-nasal drip, itchy nose, itchy mouth, itchy eyes, watery eyes, redness of the eyes, snoring, headaches, and/or sinus congestion. In those individuals with asthma whose asthma is exacerbated by pollen, chest tightness, wheezing, coughing, and/or shortness of breath may also ensue.
In addition to pollens as a source for summertime allergies, one must be cautious of flying insects, particularly if that person has a history of hives or a systemic allergic reaction resulting from an insect sting. In the Washington, DC metro area, bees, wasps, yellow jackets, white-faced hornets, and yellow-faced hornets are the major flying insects that inject venom into humans. Some individuals will naturally develop an immune response to further stings with that species of insect. As a result, when that person is subsequently stung with the insect that they are allergic to, an allergic reaction occurs which may be mild, moderate, or severe. Severe allergic reactions to flying insects due to venom allergy may be life-threatening. Anyone who has a history of hives and/or a systemic reaction to a flying insect, whether it be mild, moderate, or severe, should seek a board certified allergist to get evaluated. Allergy blood testing or allergy skin testing is warranted and depending on the results of the tests, a course of venom immunotherapy (i.e., allergy shots to venomous flying insects such as bees, wasps, yellow jackets, white-faced hornets, yellow-faced hornets) may be necessary as it is very efficacious in preventing further severe allergic reactions to flying insects if stung again. In addition, a self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine spray (e.g., Neffy) should be prescribed to anyone with a history of venom sensitivity and told to go to the closest emergency room if the epinephrine is used.
Another allergen lurking in the summertime is poison ivy. Together with poison oak and poison sumac, these plants are notorious for causing severe itching and rashes to sensitive individuals. In addition to the person who enjoys doing various activities outside, certain “outdoor” professions (e.g., construction workers, firefighters, farmers, landscapers) are at a higher risk to develop poison ivy, poison oak, poison sumac, or other plant-induced contact dermatitis than other professions where workers are primarily based indoors.
Certain groups of people or individuals are more prone to developing an allergy to sunscreen. Individuals who work outdoors on a regular basis such as farmers or construction workers, people with sun-damaged skin, and persons applying sunscreen to areas of damaged skin are more at risk. Females are more affected primarily because they are more prone to using cosmetics that can contain potentially irritating substances.
One should also remember that food allergies are always a problem, but may be a bigger problem if one is outdoors in a remote location far from an urgent care center or hospital. Thus, campers, hikers, and nature lovers should be very in tune to what foods they consume and avoiding those foods they are not supposed to eat. They should also carry their self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine spray (e.g., Neffy).
Black & Kletz Allergy has board certified allergy and immunology physicians as well as a trained staff experienced in both the diagnosis and treatment of atopic diseases such as allergic rhinitis (i.e., hay fever), allergic conjunctivitis (i.e., eye allergies), asthma, contact dermatitis (e.g., poison ivy, poison oak, poison sumac, sunscreen allergy), and food allergies. We treat both adults and children and we have 3 convenient office locations in the Washington, DC, Northern Virginia, and Maryland metropolitan area. Black & Kletz Allergy has offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. We have on-site parking at each location and the Washington, DC and McLean offices are Metro accessible. There is a free shuttle that runs between the McLean, VA office and the Spring Hill metro station on the silver line. Please call us if you, a family member, a friend, or a colleague suffer from any one of these maladies or any other allergic or immunologic problem and want to be evaluated and treated. You may also click Request an Appointment and we will respond within 24 hours of the next business day. The allergy doctors at Black & Kletz Allergy strive to keep up with the newest allergy and asthma treatment modalities so that cutting edge medicine is always at the forefront and available to our patients.
Histamine Intolerance
May 28, 2025 | Black & Kletz Allergy
 Histamine is a biogenic amine (i.e., an organic compound made up of carbon and nitrogen bonds) with several biological effects across different types of cells, mediated through the activation of histamine receptors. Histamine is normally present within mast cells and other similar cell types such as basophils. Mast cells are cells of the connective tissue that contain many granules rich in histamine and other chemicals. Histamine is also present in various types of food, such as cheese, fermented foods, wine, spinach, some types of fish and meats.
During an allergic reaction, the mast cells are triggered to release their “granules” which contain histamine and other active substances (e.g., leukotrienes, prostaglandins) into the bloodstream. It is these substances that are responsible for causing allergic symptoms which vary depending on the organ and the sensitivity of the allergic individual.
H1 (histamine 1) receptors are predominantly present in the skin and mucous membranes. When these receptors are activated by histamine, they result in allergic symptoms such as itching (i.e., pruritus), rashes, flushing, hives (i.e., urticaria), and/or soft tissue swellings (i.e., angioedema). Stimulation of the H1 receptors in the mucous membranes by histamine causes allergic symptoms such as sneezing spells, nasal congestion, runny nose, post-nasal drip, itchy throat, sinus congestion, headaches, itchy eyes, watery eyes, and/or redness of the eyes.
Allergies and excessive histamine release also play a role in asthma symptoms such as chest tightness, coughing, wheezing, and/or shortness of breath. In addition to stimulating H1 receptors, histamine also stimulates H2 receptors in the stomach and thus plays a role in acid production and digestion. Excessive levels of histamine can lead to the overproduction of stomach acid and as a result, in can cause heartburn and other gastroesophageal reflux disease (GERD) symptoms.
Histamine intolerance occurs when the body’s capacity to eliminate histamine is exceeded by the rate of histamine accumulation. In healthy individuals, the enzyme called intestinal diamine oxidase (DAO) helps eliminate histamine that was consumed from food. When the activity of DAO is inhibited by certain factors, the body’s ability to manage histamine is significantly affected. Genetic mutations causing the decreased expression of the DAO enzyme and some medications are 2 factors that can reduce the effectiveness of DAO. As a result of these factors (i.e., genetic mutations, medications), an accumulation of histamine may occur which cause symptoms that can mimic true allergic reactions. Some examples of drugs that have been found to affect DAO’s activity include verapamil, clavulanic acid, and isoniazid, among others. Certain mineral and vitamin deficiencies (e.g., vitamin C, copper) are also known to decrease DAO activity. Alcohol, on the other hand, has been found to increase the release of endogenous histamine, affecting the rate of its degradation.
Symptoms: The symptoms of histamine intolerance are varied and may involve different systems of the body.
Histamine is a biogenic amine (i.e., an organic compound made up of carbon and nitrogen bonds) with several biological effects across different types of cells, mediated through the activation of histamine receptors. Histamine is normally present within mast cells and other similar cell types such as basophils. Mast cells are cells of the connective tissue that contain many granules rich in histamine and other chemicals. Histamine is also present in various types of food, such as cheese, fermented foods, wine, spinach, some types of fish and meats.
During an allergic reaction, the mast cells are triggered to release their “granules” which contain histamine and other active substances (e.g., leukotrienes, prostaglandins) into the bloodstream. It is these substances that are responsible for causing allergic symptoms which vary depending on the organ and the sensitivity of the allergic individual.
H1 (histamine 1) receptors are predominantly present in the skin and mucous membranes. When these receptors are activated by histamine, they result in allergic symptoms such as itching (i.e., pruritus), rashes, flushing, hives (i.e., urticaria), and/or soft tissue swellings (i.e., angioedema). Stimulation of the H1 receptors in the mucous membranes by histamine causes allergic symptoms such as sneezing spells, nasal congestion, runny nose, post-nasal drip, itchy throat, sinus congestion, headaches, itchy eyes, watery eyes, and/or redness of the eyes.
Allergies and excessive histamine release also play a role in asthma symptoms such as chest tightness, coughing, wheezing, and/or shortness of breath. In addition to stimulating H1 receptors, histamine also stimulates H2 receptors in the stomach and thus plays a role in acid production and digestion. Excessive levels of histamine can lead to the overproduction of stomach acid and as a result, in can cause heartburn and other gastroesophageal reflux disease (GERD) symptoms.
Histamine intolerance occurs when the body’s capacity to eliminate histamine is exceeded by the rate of histamine accumulation. In healthy individuals, the enzyme called intestinal diamine oxidase (DAO) helps eliminate histamine that was consumed from food. When the activity of DAO is inhibited by certain factors, the body’s ability to manage histamine is significantly affected. Genetic mutations causing the decreased expression of the DAO enzyme and some medications are 2 factors that can reduce the effectiveness of DAO. As a result of these factors (i.e., genetic mutations, medications), an accumulation of histamine may occur which cause symptoms that can mimic true allergic reactions. Some examples of drugs that have been found to affect DAO’s activity include verapamil, clavulanic acid, and isoniazid, among others. Certain mineral and vitamin deficiencies (e.g., vitamin C, copper) are also known to decrease DAO activity. Alcohol, on the other hand, has been found to increase the release of endogenous histamine, affecting the rate of its degradation.
Symptoms: The symptoms of histamine intolerance are varied and may involve different systems of the body.
- Skin: pruritus, flushing, urticaria, dermatitis, and/or swelling.
- Gastrointestinal: abdominal bloating, abdominal discomfort, gas, diarrhea and/or constipation
- Respiratory: runny nose, nasal congestion, post-nasal drip, itchy throat, sneezing, sinus congestion, chest tightness, coughing, wheezing, and/or shortness of breath
- Cardiovascular: cardiac rhythm disturbances and/or blood pressure variations
- Neurological: headaches
- Restrict foods that contain high levels of histamine (e.g., seafood, fermented soybean products, aged cheese, avocado, chocolate, nuts, milk, legumes, certain fruits such as bananas). Instead, substitute histamine-rich foods with foods that are low in histamine (e.g., water, fresh juices, herbal teas, bread, rice, eggs, honey).
- Keep a food and symptom diary for 4 to 6 weeks and eliminate the suspected foods for 4 to 6 weeks and gradually reintroduce them while closely monitoring the symptoms.
- Empirical trials with antihistamine drugs, though there are no randomized trials to prove the value of this treatment in addressing histamine intolerance.
- Mast cell stabilizer medications such as cromolyn and ketotifen may be helpful in selective cases.
- The approach of supplementation with over-the-counter DAO enzyme in order to reduce excessive levels of histamine in the serum is controversial and there are no standardized guidelines available regarding the dosage.
- Supplementing with minerals and vitamins such as copper, zinc, vitamin C, and/or vitamin B6 in the case of a known deficiency, malnutrition, or restrictive diet, may be beneficial, if approved by one’s physician.
Allergies to Pollen
May 23, 2025 | Black & Kletz Allergy
 Individuals with pollen allergies may be affected throughout the year, depending on where they live or travel. In the Washington, DC, Northern Virginia, and Maryland metropolitan area, pollen allergies are bothersome to allergic individuals generally from late February through the first frost, which is usually at the end of October. In this region, trees are the first to pollinate, generally releasing tree pollen from the end of February through the end of May. The pollen peaks in April and is recognized by everyone when their cars appear “yellow” in color. The yellowish color of the cars is due to the yellow-colored tree pollen falling on and sticking to all of the motor vehicles that dominate the Washington, DC metro area. Grass pollen is released after tree pollen, usually beginning in early May and continuing until the end of the Summer. Lastly, ragweed begins to pollinate in mid-August and it lasts until the first frost, which as mentioned above, ends in late October.
It is interesting to note that a short time after the trees begin to pollinate, the cherry trees begin to flower. People both familiar and unfamiliar with allergies often misassociate the two events and wrongly conclude that the cherry trees are causing their allergies because of the timing of the two events. Notwithstanding, the media tends to get it wrong, as they tend to associate the two occurrences, which further confuses the issue. The truth is that the flowering cherry trees are not causing the hay fever (i.e., allergic rhinitis) and/or the eye allergies (allergic conjunctivitis) symptoms that the allergy sufferers are feeling, but rather it is the non-flowering trees that are the culprit. In general, flowering trees and bushes do not generally cause allergy symptoms. Individuals who have allergy symptoms from tree pollen need to inhale the pollen in order to develop the usual symptoms of allergic rhinitis. The pollen of flowering trees and bushes is heavy compared with non-flowering trees and is not wind-dispersed as a result. The pollen of non-flowering trees and bushes, on the other hand, is light in weight and thus easily dispersed by the wind. As a result, the pollen from the non-flowering trees (“ugly trees”) and bushes (“ugly bushes”) are the pollen that individuals become sensitized to and thus allergic to due to the fact that they are breathing in this pollen causing the immune system to be affected. In certain individuals, the immune system decides that it doesn’t like the tree pollen allergens and mounts a defensive response. This allergic reaction involves the production on inflammatory mediators and chemicals. These chemicals (e.g., histamine, leukotrienes, prostaglandins), which are released into the bloodstream, cause the annoying symptoms that allergic individuals dread every pollen season.
The classic symptoms experienced by most people afflicted with allergic rhinitis or hay fever may include sneezing, itchy nose, itchy throat, nasal congestion, runny nose, post-nasal drip, itchy eyes, watery eyes, redness of the eyes, itchy ears, clogged ears, sinus pressure, fatigue, headaches, snoring, coughing, chest tightness, wheezing, and/or shortness of breath.
The diagnosis of pollen allergies begins with a comprehensive history and physical examination. In the history, it is important for the allergist to ascertain if the patient experiences hay fever symptoms or worsening hay fever symptoms in the months where pollination takes place, mostly in the Spring and/or Fall. The next step is usually allergy skin testing (or blood testing) to environmental allergens in order to see if the individual is allergic and to what extent.
Avoidance measures are usually the first things recommended to a person with pollen allergies, assuming that individual wants or is able to avoid pollen. Many things can be done, but it is up to the patient to follow the recommendations by the allergist. Some of these preventive measures are as follows:
1. Turn on air conditioning.
2. Change air filters often (i.e., monthly).
3. Wash pets after they go outdoors.
4. Avoid mowing lawns and yard work or wear a filtered mask.
5. Shower, wash hair, and change clothing after coming back indoors.
6. Drive a car that has an air filter.
7. Re-circulate air in car so it doesn’t come in from the outdoors.
8. Keep sunroofs and windows closed in your vehicle.
The treatment of patients who have pollen allergies depends on the duration and the severity of symptoms. Oral antihistamines are usually the first line of defense. In individuals who need more intensive treatment, oral decongestants, nasal corticosteroids, nasal antihistamines, nasal anticholinergics, nasal mast cell stabilizers, nasal decongestants, and oral leukotriene antagonists may be utilized. In patients exhibiting ocular symptoms, eye drops containing antihistamines, leukotriene antagonists, and/or mast cell stabilizers are available. Asthmatic patients may also be treated with inhaled bronchodilators, inhaled corticosteroids, inhaled anticholinergics, and biologicals. Allergy injections (i.e., allergy shots, allergy immunotherapy, allergy desensitization, allergy hyposensitization) are very efficacious as they help in 80-85% of individuals with allergic rhinitis, allergic conjunctivitis, and/or asthma. The average patient is on allergy injections for 3-5 years.
Pollen season is upon us and the Spring pollen is blanketing the landscape in the Washington, DC metropolitan area. The board certified allergy doctors at Black & Kletz Allergy have 3 locations in the Washington, Northern Virginia, and Maryland metropolitan area. We have offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All 3 of our offices have on-site parking and the Washington, DC and McLean, VA offices are Metro accessible. The McLean office has a complementary shuttle that runs between our office and the Spring Hill metro station on the silver line. The allergy doctors of Black & Kletz Allergy diagnose and treat both adult and pediatric patients. For an appointment, please call our office or alternatively, you can click Request an Appointment and we will respond within 24 hours by the next business day. Our allergists at Black & Kletz Allergy have been helping patients with hay fever, eye allergies, asthma, sinus disease, generalized itching (pruritus), hives (i.e., urticaria), eczema (i.e., atopic dermatitis), anaphylaxis, medication allergies, food allergies, insect sting allergies, and immunological disorders for more than 5 decades. If you suffer from allergies, it is our goal to improve your quality of life by decreasing or stopping your undesirable allergy symptoms.
Individuals with pollen allergies may be affected throughout the year, depending on where they live or travel. In the Washington, DC, Northern Virginia, and Maryland metropolitan area, pollen allergies are bothersome to allergic individuals generally from late February through the first frost, which is usually at the end of October. In this region, trees are the first to pollinate, generally releasing tree pollen from the end of February through the end of May. The pollen peaks in April and is recognized by everyone when their cars appear “yellow” in color. The yellowish color of the cars is due to the yellow-colored tree pollen falling on and sticking to all of the motor vehicles that dominate the Washington, DC metro area. Grass pollen is released after tree pollen, usually beginning in early May and continuing until the end of the Summer. Lastly, ragweed begins to pollinate in mid-August and it lasts until the first frost, which as mentioned above, ends in late October.
It is interesting to note that a short time after the trees begin to pollinate, the cherry trees begin to flower. People both familiar and unfamiliar with allergies often misassociate the two events and wrongly conclude that the cherry trees are causing their allergies because of the timing of the two events. Notwithstanding, the media tends to get it wrong, as they tend to associate the two occurrences, which further confuses the issue. The truth is that the flowering cherry trees are not causing the hay fever (i.e., allergic rhinitis) and/or the eye allergies (allergic conjunctivitis) symptoms that the allergy sufferers are feeling, but rather it is the non-flowering trees that are the culprit. In general, flowering trees and bushes do not generally cause allergy symptoms. Individuals who have allergy symptoms from tree pollen need to inhale the pollen in order to develop the usual symptoms of allergic rhinitis. The pollen of flowering trees and bushes is heavy compared with non-flowering trees and is not wind-dispersed as a result. The pollen of non-flowering trees and bushes, on the other hand, is light in weight and thus easily dispersed by the wind. As a result, the pollen from the non-flowering trees (“ugly trees”) and bushes (“ugly bushes”) are the pollen that individuals become sensitized to and thus allergic to due to the fact that they are breathing in this pollen causing the immune system to be affected. In certain individuals, the immune system decides that it doesn’t like the tree pollen allergens and mounts a defensive response. This allergic reaction involves the production on inflammatory mediators and chemicals. These chemicals (e.g., histamine, leukotrienes, prostaglandins), which are released into the bloodstream, cause the annoying symptoms that allergic individuals dread every pollen season.
The classic symptoms experienced by most people afflicted with allergic rhinitis or hay fever may include sneezing, itchy nose, itchy throat, nasal congestion, runny nose, post-nasal drip, itchy eyes, watery eyes, redness of the eyes, itchy ears, clogged ears, sinus pressure, fatigue, headaches, snoring, coughing, chest tightness, wheezing, and/or shortness of breath.
The diagnosis of pollen allergies begins with a comprehensive history and physical examination. In the history, it is important for the allergist to ascertain if the patient experiences hay fever symptoms or worsening hay fever symptoms in the months where pollination takes place, mostly in the Spring and/or Fall. The next step is usually allergy skin testing (or blood testing) to environmental allergens in order to see if the individual is allergic and to what extent.
Avoidance measures are usually the first things recommended to a person with pollen allergies, assuming that individual wants or is able to avoid pollen. Many things can be done, but it is up to the patient to follow the recommendations by the allergist. Some of these preventive measures are as follows:
1. Turn on air conditioning.
2. Change air filters often (i.e., monthly).
3. Wash pets after they go outdoors.
4. Avoid mowing lawns and yard work or wear a filtered mask.
5. Shower, wash hair, and change clothing after coming back indoors.
6. Drive a car that has an air filter.
7. Re-circulate air in car so it doesn’t come in from the outdoors.
8. Keep sunroofs and windows closed in your vehicle.
The treatment of patients who have pollen allergies depends on the duration and the severity of symptoms. Oral antihistamines are usually the first line of defense. In individuals who need more intensive treatment, oral decongestants, nasal corticosteroids, nasal antihistamines, nasal anticholinergics, nasal mast cell stabilizers, nasal decongestants, and oral leukotriene antagonists may be utilized. In patients exhibiting ocular symptoms, eye drops containing antihistamines, leukotriene antagonists, and/or mast cell stabilizers are available. Asthmatic patients may also be treated with inhaled bronchodilators, inhaled corticosteroids, inhaled anticholinergics, and biologicals. Allergy injections (i.e., allergy shots, allergy immunotherapy, allergy desensitization, allergy hyposensitization) are very efficacious as they help in 80-85% of individuals with allergic rhinitis, allergic conjunctivitis, and/or asthma. The average patient is on allergy injections for 3-5 years.
Pollen season is upon us and the Spring pollen is blanketing the landscape in the Washington, DC metropolitan area. The board certified allergy doctors at Black & Kletz Allergy have 3 locations in the Washington, Northern Virginia, and Maryland metropolitan area. We have offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All 3 of our offices have on-site parking and the Washington, DC and McLean, VA offices are Metro accessible. The McLean office has a complementary shuttle that runs between our office and the Spring Hill metro station on the silver line. The allergy doctors of Black & Kletz Allergy diagnose and treat both adult and pediatric patients. For an appointment, please call our office or alternatively, you can click Request an Appointment and we will respond within 24 hours by the next business day. Our allergists at Black & Kletz Allergy have been helping patients with hay fever, eye allergies, asthma, sinus disease, generalized itching (pruritus), hives (i.e., urticaria), eczema (i.e., atopic dermatitis), anaphylaxis, medication allergies, food allergies, insect sting allergies, and immunological disorders for more than 5 decades. If you suffer from allergies, it is our goal to improve your quality of life by decreasing or stopping your undesirable allergy symptoms.
Is Primatene Mist Good for Asthma?
April 15, 2025 | Black & Kletz Allergy
There are a few over-the-counter (OTC) medications that some patients with asthma and other respiratory conditions occasionally use. One of them is an inhaler called Primatene Mist. Primatene Mist contains epinephrine (i.e., adrenaline) in an inhalable form. Though it is the same drug that is in an EpiPen, Auvi-Q, Adrenaclick, and other self-injectable epinephrine devices as well as the nasal spray, Neffy, used to treat acute allergic emergencies such as anaphylaxis, Primatene Mist does not help in those situations and should not be used. Although Primatene Mist became available in 1967, the FDA took it off the market in 2011, as it contained propellants called chlorofluorocarbons (CFC’s) which are harmful to the environment as they deplete ozone from the atmosphere. However, Primatene mist was recently reintroduced into the market with a newer propellant called hydrofluoroalkanes (HFA’s), which are environment friendly. Primatene Mist temporarily opens up the airways in the lungs thus offering a very short-term relief from shortness of breath and/or wheezing. It is approved only for individuals with an established prior diagnosis of asthma. It is used for the temporary relief of mild symptoms of intermittent asthma in patients aged 12 years or older and should not be used as a replacement for prescription asthma medications. Primatene Mist can do more harm than good if used for a chronic cough, for instance, without a known cause.
The risks of Primatene Mist usage include masking of the symptoms without addressing the underlying cause. The symptoms of chest tightness, wheezing, cough, and/or shortness of breath should lead to the proper evaluation in order to establish the reason behind the symptoms.
In cases of asthma, the underlying cause could be long-standing inflammation of the lungs. Proper evaluation and management should include the assessment of the lung function in addition to trying to control the causative factors. Uncontrolled inflammation can result in damage to the lung tissues and a reduction in lung capacity over time, which can be irreversible. Several deaths are reported each year in the USA due to uncontrolled asthma. Deaths also occur in cases of mild asthma with acute exacerbations.
Primatene Mist is also associated with undesirable side effects such as palpitations, increase in blood pressure, nervousness, etc. In the elderly and in individuals with certain conditions such as heart problems, Primatene Mist may be harmful as epinephrine may worsen their underlying conditions. There is also concern for misuse or abuse. Primatene Mist may make the individual feel better temporarily when in fact the underlying reason for the exacerbation of the asthma goes unchecked, leading to a worse outcome overall because the individual did not seek the proper care. Albuterol, a prescribed alternative medication, is typically used for the quick relief of asthma symptoms. It is a bronchodilator which acts by relaxing the muscles around the airways so that they can open up better making it easier to breath. Primatene Mist is less potent and has a much shorter duration of action than albuterol, and thus not preferred.
Primatene Mist is not recommended for severe asthma or as a long-term treatment. It should not be used in children under the age of 12 years old. There is a defined role for albuterol in relieving symptoms while also controls the underlying cause(s) with anti-inflammatory medications. In fact, there is an albuterol inhaler that has a corticosteroid added to it in order to give the medication an anti-inflammatory benefit when treating the symptoms of asthma. This medication is called AirSupra and it contains both albuterol and the corticosteroid called budesonide. It should also be noted that the national and international guidelines by organizations such as the National Institutes of Health (NIH) and the Global Initiative for Asthma (GINA) do not recommend using Primatene Mist.
The board certified allergists at Black & Kletz Allergy are always available for our patients to ask any questions that they may have regarding asthma or allergies. We have been treating adult and pediatric patients with asthma for more than 50 years. In addition, we diagnose and treat individuals with allergic rhinitis (i.e., hay fever), allergic skin conditions such as urticaria (i.e., hives) and atopic dermatitis (i.e., eczema), eosinophilic disorders, insect sting allergies, medication allergies, and immune disorders. We have 3 office locations in the Washington, DC, Northern Virginia, and Maryland metropolitan area with offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All of our offices offer on-site parking and the Washington, DC and McLean, VA offices are Metro accessible. There is a free shuttle that runs between our McLean, VA office and the Spring Hill metro station on the silver line. If you would like to be evaluated today for asthma or any other allergic or immunologic problem, please call us today. You may also click Request an Appointment instead and we will respond to your request within 24 hours by the next business day. The allergy specialists at Black & Kletz Allergy pride themselves in providing the highest quality asthma and allergy care in the Washington, DC metro area.
Although Primatene Mist became available in 1967, the FDA took it off the market in 2011, as it contained propellants called chlorofluorocarbons (CFC’s) which are harmful to the environment as they deplete ozone from the atmosphere. However, Primatene mist was recently reintroduced into the market with a newer propellant called hydrofluoroalkanes (HFA’s), which are environment friendly. Primatene Mist temporarily opens up the airways in the lungs thus offering a very short-term relief from shortness of breath and/or wheezing. It is approved only for individuals with an established prior diagnosis of asthma. It is used for the temporary relief of mild symptoms of intermittent asthma in patients aged 12 years or older and should not be used as a replacement for prescription asthma medications. Primatene Mist can do more harm than good if used for a chronic cough, for instance, without a known cause.
The risks of Primatene Mist usage include masking of the symptoms without addressing the underlying cause. The symptoms of chest tightness, wheezing, cough, and/or shortness of breath should lead to the proper evaluation in order to establish the reason behind the symptoms.
In cases of asthma, the underlying cause could be long-standing inflammation of the lungs. Proper evaluation and management should include the assessment of the lung function in addition to trying to control the causative factors. Uncontrolled inflammation can result in damage to the lung tissues and a reduction in lung capacity over time, which can be irreversible. Several deaths are reported each year in the USA due to uncontrolled asthma. Deaths also occur in cases of mild asthma with acute exacerbations.
Primatene Mist is also associated with undesirable side effects such as palpitations, increase in blood pressure, nervousness, etc. In the elderly and in individuals with certain conditions such as heart problems, Primatene Mist may be harmful as epinephrine may worsen their underlying conditions. There is also concern for misuse or abuse. Primatene Mist may make the individual feel better temporarily when in fact the underlying reason for the exacerbation of the asthma goes unchecked, leading to a worse outcome overall because the individual did not seek the proper care. Albuterol, a prescribed alternative medication, is typically used for the quick relief of asthma symptoms. It is a bronchodilator which acts by relaxing the muscles around the airways so that they can open up better making it easier to breath. Primatene Mist is less potent and has a much shorter duration of action than albuterol, and thus not preferred.
Primatene Mist is not recommended for severe asthma or as a long-term treatment. It should not be used in children under the age of 12 years old. There is a defined role for albuterol in relieving symptoms while also controls the underlying cause(s) with anti-inflammatory medications. In fact, there is an albuterol inhaler that has a corticosteroid added to it in order to give the medication an anti-inflammatory benefit when treating the symptoms of asthma. This medication is called AirSupra and it contains both albuterol and the corticosteroid called budesonide. It should also be noted that the national and international guidelines by organizations such as the National Institutes of Health (NIH) and the Global Initiative for Asthma (GINA) do not recommend using Primatene Mist.
The board certified allergists at Black & Kletz Allergy are always available for our patients to ask any questions that they may have regarding asthma or allergies. We have been treating adult and pediatric patients with asthma for more than 50 years. In addition, we diagnose and treat individuals with allergic rhinitis (i.e., hay fever), allergic skin conditions such as urticaria (i.e., hives) and atopic dermatitis (i.e., eczema), eosinophilic disorders, insect sting allergies, medication allergies, and immune disorders. We have 3 office locations in the Washington, DC, Northern Virginia, and Maryland metropolitan area with offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All of our offices offer on-site parking and the Washington, DC and McLean, VA offices are Metro accessible. There is a free shuttle that runs between our McLean, VA office and the Spring Hill metro station on the silver line. If you would like to be evaluated today for asthma or any other allergic or immunologic problem, please call us today. You may also click Request an Appointment instead and we will respond to your request within 24 hours by the next business day. The allergy specialists at Black & Kletz Allergy pride themselves in providing the highest quality asthma and allergy care in the Washington, DC metro area.
Pollen Food Allergy Syndrome Revisited
April 10, 2025 | Black & Kletz Allergy
 Pollen food allergy syndrome (PFAS), also known as oral allergy syndrome, is a condition in which there is first a “sensitization” of the immune system to various pollens and subsequent “reactions” when exposed to these pollens. Secondly, there is a similarity of the protein allergens in the pollen and the protein allergens of certain raw or fresh fruits and/or vegetables. The individual’s immune system, which has been previously sensitized to pollen, will also react to the similarly structured proteins in the raw or fresh fruits and/or vegetables. As a result, when a person who has a pollen allergy (usually trees and/or weeds) eats certain raw or fresh fruits and/or vegetables, that individual’s immune system “thinks” that it is being exposed to pollen proteins when in fact it is being exposed to fruit and/or vegetable proteins that have a very similar chemical structure to the pollen proteins. The body in turn reacts to the fresh fruit and/or vegetable proteins in a similar fashion as a typical allergic reaction but is usually more localized to where the food makes direct contact, such as the lips, tongue, palate, ears, gums, and/or throat. Essentially, there is a cross-reaction to the fresh fruit and/or vegetable because that food is mistaken for pollen and thus reacts in a similar way except the reaction is mostly where contact occurs between the food and the mouth. Note that if the fruit or vegetable is cooked, the pollen food allergy reaction does not usually take place because the heating of the fruit and/or vegetable denatures the protein resulting in the immune system not recognizing this denatured protein anymore because the altered structure of the protein does not look like the pollen protein (allergen) anymore.
The symptoms experienced by the individual who has pollen food allergy syndrome typically includes itching of the lips, tongue, palate, ears, gums, and/or throat after eating raw fresh fruits and/or vegetables. Swelling of the lips, tongue, and uvula, as well as a tightness of the throat feeling may occur in some individuals. Very rarely, a more severe allergic reaction such as hives, generalized itching, wheezing, shortness of breath, drop in blood pressure, and/or anaphylaxis can occur. In these patients, a self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine device (e.g., Neffy) is prescribed and individuals are told to go to the closest emergency room if the self-injectable epinephrine device or epinephrine nasal spray is used. It should be noted that certain nuts in certain individuals may also cause pollen food allergy syndrome symptoms. However, it must be stressed that most nut allergy reactions are not a result of pollen food allergy syndrome but rather a true IgE-mediated Type I allergic reaction which may result in a reaction that is severe and even life-threatening.
About 33% of people who have seasonal allergic rhinitis (i.e., hay fever) have pollen food allergy syndrome. In adults, close to 55% of all food allergic reactions are due to a cross-reaction between a food and a pollen. Luckily however, the reaction experienced by most individuals who have pollen food allergy syndrome is minor and self-limited. The symptoms of pollen food allergy syndrome usually occur within minutes of ingesting the food. In pollen food allergy syndrome, in general, once the allergen reaches the stomach, it is broken down by the stomach acid, and the allergic reaction does not progress further. Although the symptoms can occur at any time during the year, pollen food allergy syndrome symptoms most often occur during the corresponding pollen season. The allergenic proteins associated with pollen food allergy syndrome are usually destroyed by cooking the food. As a result, most reactions in patients with pollen food allergy syndrome are caused by eating “raw” or “fresh” fruits and/ or vegetables. The main exceptions to this are celery and nuts, which may cause reactions even after being cooked.
Certain pollens are more likely to cross-react with certain raw or fresh fruits, vegetables, and/or nuts. The list below demonstrates the cross-reactivity that may occur between common pollens and raw or fresh fruits, vegetables, and/or nuts:
Pollen food allergy syndrome (PFAS), also known as oral allergy syndrome, is a condition in which there is first a “sensitization” of the immune system to various pollens and subsequent “reactions” when exposed to these pollens. Secondly, there is a similarity of the protein allergens in the pollen and the protein allergens of certain raw or fresh fruits and/or vegetables. The individual’s immune system, which has been previously sensitized to pollen, will also react to the similarly structured proteins in the raw or fresh fruits and/or vegetables. As a result, when a person who has a pollen allergy (usually trees and/or weeds) eats certain raw or fresh fruits and/or vegetables, that individual’s immune system “thinks” that it is being exposed to pollen proteins when in fact it is being exposed to fruit and/or vegetable proteins that have a very similar chemical structure to the pollen proteins. The body in turn reacts to the fresh fruit and/or vegetable proteins in a similar fashion as a typical allergic reaction but is usually more localized to where the food makes direct contact, such as the lips, tongue, palate, ears, gums, and/or throat. Essentially, there is a cross-reaction to the fresh fruit and/or vegetable because that food is mistaken for pollen and thus reacts in a similar way except the reaction is mostly where contact occurs between the food and the mouth. Note that if the fruit or vegetable is cooked, the pollen food allergy reaction does not usually take place because the heating of the fruit and/or vegetable denatures the protein resulting in the immune system not recognizing this denatured protein anymore because the altered structure of the protein does not look like the pollen protein (allergen) anymore.
The symptoms experienced by the individual who has pollen food allergy syndrome typically includes itching of the lips, tongue, palate, ears, gums, and/or throat after eating raw fresh fruits and/or vegetables. Swelling of the lips, tongue, and uvula, as well as a tightness of the throat feeling may occur in some individuals. Very rarely, a more severe allergic reaction such as hives, generalized itching, wheezing, shortness of breath, drop in blood pressure, and/or anaphylaxis can occur. In these patients, a self-injectable epinephrine device (e.g., EpiPen, Auvi-Q, Adrenaclick) or intranasal epinephrine device (e.g., Neffy) is prescribed and individuals are told to go to the closest emergency room if the self-injectable epinephrine device or epinephrine nasal spray is used. It should be noted that certain nuts in certain individuals may also cause pollen food allergy syndrome symptoms. However, it must be stressed that most nut allergy reactions are not a result of pollen food allergy syndrome but rather a true IgE-mediated Type I allergic reaction which may result in a reaction that is severe and even life-threatening.
About 33% of people who have seasonal allergic rhinitis (i.e., hay fever) have pollen food allergy syndrome. In adults, close to 55% of all food allergic reactions are due to a cross-reaction between a food and a pollen. Luckily however, the reaction experienced by most individuals who have pollen food allergy syndrome is minor and self-limited. The symptoms of pollen food allergy syndrome usually occur within minutes of ingesting the food. In pollen food allergy syndrome, in general, once the allergen reaches the stomach, it is broken down by the stomach acid, and the allergic reaction does not progress further. Although the symptoms can occur at any time during the year, pollen food allergy syndrome symptoms most often occur during the corresponding pollen season. The allergenic proteins associated with pollen food allergy syndrome are usually destroyed by cooking the food. As a result, most reactions in patients with pollen food allergy syndrome are caused by eating “raw” or “fresh” fruits and/ or vegetables. The main exceptions to this are celery and nuts, which may cause reactions even after being cooked.
Certain pollens are more likely to cross-react with certain raw or fresh fruits, vegetables, and/or nuts. The list below demonstrates the cross-reactivity that may occur between common pollens and raw or fresh fruits, vegetables, and/or nuts:
- Alder pollen: Apples, cherries, peaches, pears, almonds, celery, hazelnuts, parsley
- Birch pollen: Apples, avocados, apricots, carrots, bananas, cherries, figs, nectarines, kiwis, peaches, pears, plums, prunes, strawberries, almonds, hazelnuts, peanuts, coriander, celery, chicory, fennel, potatoes, parsley, parsnips, peppers, wheat, soy
- Grass pollen: Tomatoes, oranges, melons, figs
- Mugwort pollen (i.e., celery-mugwort-spice-syndrome)
: Celery, carrots, fennel, coriander, parsley, peppers, sunflower - Ragweed pollen: Melons (e.g., honeydew, cantaloupe, watermelon), bananas, artichokes, cucumbers, zucchini, Echinacea, dandelions, chamomile tea, hibiscus tea
Tree Pollen Allergies Update in the Washington, DC Area
March 25, 2025 | Black & Kletz Allergy
 Spring is here! This means that quite a few Washingtonians will be pretty miserable as they will be suffering from hay fever (i.e., allergic rhinitis). In the early Spring, tree pollen is mostly to blame for the annoying symptoms that cause hay fever. Other than tree pollen, molds are also a common environmental allergen that plays havoc with allergy sufferers. It should be noted that tree pollen can exacerbate asthma as well as cause allergic eye symptoms (i.e., allergic conjunctivitis).
In the Washington, DC, Northern Virginia, and Maryland metropolitan area, trees typically begin to pollinate at the end of February, peak in mid- to late-April and continue to pollinate through late May and occasionally through early June. The first trees to pollinate in the Washington, DC metro area cedar, birch, maple, poplar, elm, and alder. Later in the Spring season, the principal tree that causes difficulties for people with tree pollen allergies is the oak tree. In addition to oak tree, however, other tress that pollinate during the same time as oak trees include hickory, walnut, and pine trees.
Tree pollen, as well as other pollens (e.g., grasses, weeds), pollinates by releasing its pollen into the air. In general, most non-flowering trees have pollen that is light in weight. When the pollen in released into the air, it is carried by the wind and the pollen grains land on other trees. It is this cross-pollination that allows trees to reproduce. Although it is good for the trees, it is not so good for allergy patients. If outdoors when tree pollination takes place, a tree-sensitive individual will breathe in the pollen-infested air which will cause that person to exhibit allergic rhinitis symptoms.
The symptoms of tree pollen allergy may include sneezing, runny nose, nasal congestion, post-nasal drip (which may cause a sore throat or cough), itchy throat, itchy nose, itchy eyes, watery eyes, red eyes, puffy eyes, sinus pressure and/or pain, snoring, chest tightness, wheezing, cough, and/or shortness of breath. Tree pollen as well as other environmental allergens (e.g., grasses, weeds, molds, dust mites, pets, cockroaches) may also exacerbate asthma in patients with this condition.
An interesting fact regarding flowers or flowering trees is that they generally do not cause hay fever symptoms because the pollen is too heavy, and as a result, the pollen is not wind-disbursed. If they are too heavy to be transported in the air to other flowering trees, then one generally does not become sensitized to the pollen because they are not breathing in this heavier pollen. It is thought that the flowers are an adaptation over millions of years in order to attract bees. By design, bees have taken over for cross-pollinating flowering trees by landing on the flowers and then flying to other flowering trees. When the bee lands on the flower, tree pollen gets stuck to their abdomen. When they fly to another flowering tree, the pollen on its abdomen rubs off on the flowers allowing cross-pollination of that species of tree.
The diagnosis of tree pollen allergy begins with a comprehensive history and physical examination. Allergy skin testing or blood testing (in select individuals) is usually performed in order to identify a tree allergy.
Once a diagnosis of tree pollen allergy is confirmed, avoidance of tree pollen and prophylactic measures should be tried, if at all possible. If one goes outside, take a shower, wash one’s hair, and change one’s clothing when returning home in order to lessen pollen exposure. It is wise to turn on the air conditioner and change air filters regularly (approximately once a month). In addition, close one’s windows and sunroof and re-circulate the air in the car in order to avoid outside air from entering the vehicle. At home, avoid mowing one’s lawn and yard work. If these tasks must be done, where a filtration mask to lessen exposure to tree pollen. Also avoid close contact with a pet that goes outside since they carry tree pollen on their coats. If they go outdoors, wash the per regularly. Check pollen counts every day and click Today’s Pollen Count on our website to see the daily pollen count. Stay inside whenever possible during the Spring, especially when the tree pollen count is high. If you must go outside, try to avoid exercising outdoors in the early mornings because pollen tends to be released more during that time frame. Avoid wearing contact lenses which may trap the tree pollen in one’s eyes. It is important to know that rain washes tree pollen from the air causing the pollen counts to be lower on wet cooler days.
The treatment of tree pollen allergy, other than trying to avoid exposure, usually begins with taking allergy medications. There are also a multitude of medications available that may help diminish allergy symptoms. Some of these medications may include antihistamines, decongestants, leukotriene inhibitors, nasal corticosteroids, nasal antihistamines, nasal mast cell stabilizers, nasal anticholinergics, ocular antihistamines, and/or ocular mast cell stabilizers. Allergy shots (i.e., allergy immunotherapy, allergy desensitization, allergy hyposensitization) are a very efficacious treatment modality in patients with all types of environmental allergies, including tree pollen allergies. They work in 80-85% of patients that take them. It is also helpful in the treatment of allergic conjunctivitis as well as asthma.
The board certified allergy specialists at Black & Kletz Allergy have been treating individuals with tree pollen allergies for over 50 years. If you suffer from any of the symptoms above in the Spring, please call our office for an allergy consultation in order for us to determine if you have tree or other allergies that may cause any of the symptoms above. We have 3 offices in the Washington, DC, Northern Virginia, and Maryland metropolitan area with office locations in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. We offer on-site parking at each location and the Washington, DC and McLean, VA offices are Metro accessible. There is a free shuttle that runs between the McLean, VA office and the Spring Hill metro station on the silver line. Black & Kletz Allergy specializes in treatment of both adult and pediatric patients. Alternatively, to schedule an appointment, you may click Request an Appointment and we will respond within 24 hours by the next business day. The allergy doctors at Black & Kletz Allergy pride themselves in providing superior allergy and asthma care in a specialized and caring environment.
Spring is here! This means that quite a few Washingtonians will be pretty miserable as they will be suffering from hay fever (i.e., allergic rhinitis). In the early Spring, tree pollen is mostly to blame for the annoying symptoms that cause hay fever. Other than tree pollen, molds are also a common environmental allergen that plays havoc with allergy sufferers. It should be noted that tree pollen can exacerbate asthma as well as cause allergic eye symptoms (i.e., allergic conjunctivitis).
In the Washington, DC, Northern Virginia, and Maryland metropolitan area, trees typically begin to pollinate at the end of February, peak in mid- to late-April and continue to pollinate through late May and occasionally through early June. The first trees to pollinate in the Washington, DC metro area cedar, birch, maple, poplar, elm, and alder. Later in the Spring season, the principal tree that causes difficulties for people with tree pollen allergies is the oak tree. In addition to oak tree, however, other tress that pollinate during the same time as oak trees include hickory, walnut, and pine trees.
Tree pollen, as well as other pollens (e.g., grasses, weeds), pollinates by releasing its pollen into the air. In general, most non-flowering trees have pollen that is light in weight. When the pollen in released into the air, it is carried by the wind and the pollen grains land on other trees. It is this cross-pollination that allows trees to reproduce. Although it is good for the trees, it is not so good for allergy patients. If outdoors when tree pollination takes place, a tree-sensitive individual will breathe in the pollen-infested air which will cause that person to exhibit allergic rhinitis symptoms.
The symptoms of tree pollen allergy may include sneezing, runny nose, nasal congestion, post-nasal drip (which may cause a sore throat or cough), itchy throat, itchy nose, itchy eyes, watery eyes, red eyes, puffy eyes, sinus pressure and/or pain, snoring, chest tightness, wheezing, cough, and/or shortness of breath. Tree pollen as well as other environmental allergens (e.g., grasses, weeds, molds, dust mites, pets, cockroaches) may also exacerbate asthma in patients with this condition.
An interesting fact regarding flowers or flowering trees is that they generally do not cause hay fever symptoms because the pollen is too heavy, and as a result, the pollen is not wind-disbursed. If they are too heavy to be transported in the air to other flowering trees, then one generally does not become sensitized to the pollen because they are not breathing in this heavier pollen. It is thought that the flowers are an adaptation over millions of years in order to attract bees. By design, bees have taken over for cross-pollinating flowering trees by landing on the flowers and then flying to other flowering trees. When the bee lands on the flower, tree pollen gets stuck to their abdomen. When they fly to another flowering tree, the pollen on its abdomen rubs off on the flowers allowing cross-pollination of that species of tree.
The diagnosis of tree pollen allergy begins with a comprehensive history and physical examination. Allergy skin testing or blood testing (in select individuals) is usually performed in order to identify a tree allergy.
Once a diagnosis of tree pollen allergy is confirmed, avoidance of tree pollen and prophylactic measures should be tried, if at all possible. If one goes outside, take a shower, wash one’s hair, and change one’s clothing when returning home in order to lessen pollen exposure. It is wise to turn on the air conditioner and change air filters regularly (approximately once a month). In addition, close one’s windows and sunroof and re-circulate the air in the car in order to avoid outside air from entering the vehicle. At home, avoid mowing one’s lawn and yard work. If these tasks must be done, where a filtration mask to lessen exposure to tree pollen. Also avoid close contact with a pet that goes outside since they carry tree pollen on their coats. If they go outdoors, wash the per regularly. Check pollen counts every day and click Today’s Pollen Count on our website to see the daily pollen count. Stay inside whenever possible during the Spring, especially when the tree pollen count is high. If you must go outside, try to avoid exercising outdoors in the early mornings because pollen tends to be released more during that time frame. Avoid wearing contact lenses which may trap the tree pollen in one’s eyes. It is important to know that rain washes tree pollen from the air causing the pollen counts to be lower on wet cooler days.
The treatment of tree pollen allergy, other than trying to avoid exposure, usually begins with taking allergy medications. There are also a multitude of medications available that may help diminish allergy symptoms. Some of these medications may include antihistamines, decongestants, leukotriene inhibitors, nasal corticosteroids, nasal antihistamines, nasal mast cell stabilizers, nasal anticholinergics, ocular antihistamines, and/or ocular mast cell stabilizers. Allergy shots (i.e., allergy immunotherapy, allergy desensitization, allergy hyposensitization) are a very efficacious treatment modality in patients with all types of environmental allergies, including tree pollen allergies. They work in 80-85% of patients that take them. It is also helpful in the treatment of allergic conjunctivitis as well as asthma.
The board certified allergy specialists at Black & Kletz Allergy have been treating individuals with tree pollen allergies for over 50 years. If you suffer from any of the symptoms above in the Spring, please call our office for an allergy consultation in order for us to determine if you have tree or other allergies that may cause any of the symptoms above. We have 3 offices in the Washington, DC, Northern Virginia, and Maryland metropolitan area with office locations in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. We offer on-site parking at each location and the Washington, DC and McLean, VA offices are Metro accessible. There is a free shuttle that runs between the McLean, VA office and the Spring Hill metro station on the silver line. Black & Kletz Allergy specializes in treatment of both adult and pediatric patients. Alternatively, to schedule an appointment, you may click Request an Appointment and we will respond within 24 hours by the next business day. The allergy doctors at Black & Kletz Allergy pride themselves in providing superior allergy and asthma care in a specialized and caring environment.
Food Protein-Induced Enterocolitis Syndrome (FPIES)
March 20, 2025 | Black & Kletz Allergy
 Food protein-induced enterocolitis syndrome (FPIES) is a rare condition that causes gastrointestinal symptoms several hours after consumption of certain foods by an individual who has an intolerance to that food. The prevalence rate in the United States is approximately 0.5%. The most common types of food allergy in children and adults are mediated by an antibody called IgE. Food allergies may result in adverse reactions which in some cases may be very severe and even life-threatening in some that may occur within minutes of ingestion of the offending food. The IgE antibodies are specific to the food that causes the reaction.
However, in individuals with FPIES, the intolerance to the food is not caused by IgE antibodies and the symptoms are usually delayed in onset. It should however be noted that on occasion, FPIES may coexist with IgE mediated classic food allergies.
In infants and children with FPIES, the most common foods that trigger gastrointestinal symptoms are milk, soy, oats, rice, and eggs. For exclusively breastfed infants, FPIES reactions generally only begin when other foods are added to their diet. For bottle-fed infants, FPIES reactions may begin in the first few months of life. The most common trigger in adults with FPIES is seafood, particularly shellfish.
Symptoms:
Food protein-induced enterocolitis syndrome (FPIES) is a rare condition that causes gastrointestinal symptoms several hours after consumption of certain foods by an individual who has an intolerance to that food. The prevalence rate in the United States is approximately 0.5%. The most common types of food allergy in children and adults are mediated by an antibody called IgE. Food allergies may result in adverse reactions which in some cases may be very severe and even life-threatening in some that may occur within minutes of ingestion of the offending food. The IgE antibodies are specific to the food that causes the reaction.
However, in individuals with FPIES, the intolerance to the food is not caused by IgE antibodies and the symptoms are usually delayed in onset. It should however be noted that on occasion, FPIES may coexist with IgE mediated classic food allergies.
In infants and children with FPIES, the most common foods that trigger gastrointestinal symptoms are milk, soy, oats, rice, and eggs. For exclusively breastfed infants, FPIES reactions generally only begin when other foods are added to their diet. For bottle-fed infants, FPIES reactions may begin in the first few months of life. The most common trigger in adults with FPIES is seafood, particularly shellfish.
Symptoms:
- Vomiting, typically occurring 1 - 4 hours after ingestion
- Diarrhea
- Blood and mucus in the stools
- Dehydration
- Fatigue
- Changes in blood pressure and body temperature
- In most cases, allergy skin prick and/or allergy blood tests will be negative, as this condition is not mediated by the IgE antibody.
- The diagnosis is most often established based on a comprehensive history and physical examination, after excluding other common conditions.
- Blood tests usually reveal the immune system’s response to stress, such as infections.
- Confirmation of the diagnosis often requires an oral challenge with the suspected food under close monitoring in a controlled environment in an attempt to trigger the symptoms.
- Children can rapidly become dehydrated following vomiting and diarrhea which may lead to a shock-like condition. Immediate rehydration intravenously and/or orally can be lifesaving.
- Zofran (ondansetron), an oral medication that controls nausea and vomiting, is sometimes useful in older children and adults.
- Breastfeeding infants, who begin exhibiting FPIES symptoms when solids are introduced into their diets, may need to continue exclusive breastfeeding for several more months.
- Infants who have reacted to dairy and/or soy-based infant formulas often need to be switched to hypoallergenic or elemental formulas.
- Oral corticosteroids may sometimes be prescribed in order to reduce the immune reaction as a short term measure.
- In older children and adults, eliminating one or more foods based on the clinical history and/or oral challenges may be warranted for prolonged periods.
- Foods are gradually reintroduced into the diet, one at a time, based on the results of oral challenges.
- Many children outgrow FPIES and will be able to tolerate the foods spontaneously by the age of 3.
- Dairy is usually tolerated much earlier than rice and other cereals. Seafood may take several years to outgrow.
- Some children continue to experience FPIES symptoms into adolescence and into adulthood.
- As the underlying pathology is not yet fully understood, no curative treatments are available at this time.
Update on Angioedema (Swelling Episodes)
February 13, 2025 | Black & Kletz Allergy
 Some individuals have episodes of swelling or “angioedema” of various tissues that may occur without any known rhyme or reason. They may have 1 episode or they may have multiple or recurrent episodes. Most people with this condition are very surprised and nervous when they notice an area of their body swelling up right in front of their eyes. The swelling can occur on any part of the body or even internally. They may occur by themselves or they may be accompanied with hives (i.e., urticaria) and/or generalized itching (i.e., pruritus). The severity of the swelling can range from very mild to extremely severe. The swelling occurs because there is seepage of fluid through small blood vessel walls which in turn results in soft tissue swelling.
The allergic causes of angioedema are varied and may include the following:
Some individuals have episodes of swelling or “angioedema” of various tissues that may occur without any known rhyme or reason. They may have 1 episode or they may have multiple or recurrent episodes. Most people with this condition are very surprised and nervous when they notice an area of their body swelling up right in front of their eyes. The swelling can occur on any part of the body or even internally. They may occur by themselves or they may be accompanied with hives (i.e., urticaria) and/or generalized itching (i.e., pruritus). The severity of the swelling can range from very mild to extremely severe. The swelling occurs because there is seepage of fluid through small blood vessel walls which in turn results in soft tissue swelling.
The allergic causes of angioedema are varied and may include the following:
- Allergies to Food – Peanuts (legumes), tree nuts, fish, shellfish, eggs, milk, etc.
- Insect Sting Allergies – Honey bees, wasps, yellow jackets, hornets, fire ants, etc.
- Medication Allergies – Penicillin, sulfa, erythromycin, tetracycline, aspirin, nonsteroidal anti-inflammatory drugs (NDAIDS), vaccines, etc.
- Natural Rubber Latex – Gloves, balloons, condoms, catheters, dental dams, etc.
- Autoimmune Disorders – Rheumatoid arthritis, systemic lupus erythematosus, Sjögren’s syndrome, polymyositis, scleroderma, Grave’s disease, Hashimoto’s thyroiditis, etc.
- Certain cancers
- Infections – Hepatitis B, syphilis, etc.
- Angiotensin II Receptor Antagonists - Diovan (valsartan), Cozaar (losartan), Atacand (candesartan), Micardis (telmisartan), Benicar (olmesartan), Avapro (irbesartan), etc.
- Proton Pump Inhibitors - Prevacid (lansoprazole), Nexium (esomeprazole), Dexilant (dexlansoprazole), Prilosec (omeprazole), Aciphex (rabeprazole), Protonix (pantoprazole), etc.
- Angiotensin Converting Enzyme (ACE) Inhibitors - Altace (ramipril), Vasotec (enalapril), Zestril (Lisinopril), Capoten (Captopril), Lotensin (benazepril), Accupril (quinapril), etc.
- Selective Serotonin Reuptake Inhibitors (SSRI’s) - Lexapro (escitalopram), Prozac (fluoxetine), Zoloft (sertraline), Paxil (paroxetine), Luvox (fluvoxamine), Celexa (citalopram), etc.
- Statins - Zocor (simvastatin), Lipitor (atorvastatin), Pravachol (pravastatin), Crestor (rosuvastatin), Lescol (fluvastatin), Mevacor (lovastatin), etc.












