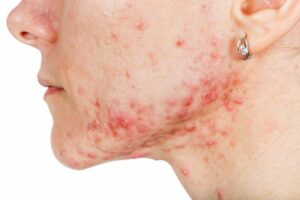
The exact cause of prurigo nodularis is unknown, but altered function of the immune system and nerves in the skin is believed to be associated with heightened sensations of itchiness (i.e., pruritus) that leads to frequent scratching. Frequent scratching and picking of the skin are also thought to contribute to further lesion formation and thickening seen in the disease.
Prurigo nodularis can occur at any age but is more common in the elderly. When it occurs in younger patients, it is more likely to be associated with inflammatory skin diseases, usually eczema (i.e., atopic dermatitis). Prurogo nodularis is also more likely to manifest in patients with other underlying medical conditions that affect multiple body systems, such as cancer, diabetes, chronic kidney disease, and HIV infection. Prurigo nodularis is not hereditary or contagious.
The rash and itching can be episodic or continuous, lasting for several months in some individuals. It is typically worsened by sweat, heat, synthetic clothing, and/or stress. The rash can range in severity from just a few to several hundred lesions. The lesions can range in size from 0.2 inches to 0.8 inches wide and can appear as firm, dome-shaped papules, nodules, or plaques. Lesions can be flesh-colored, pink, red, brown, or black in color.
Diagnosis:
- The characteristic appearance and distribution of the lesions, the chronicity, and association with other systemic disorders provide clues to the diagnosis of prurigo nodularis.
- The confirmation of the diagnosis is established by biopsy of the skin lesions and examination of them under a microscope. It usually reveals thickening of different areas of the outermost layer of the skin (i.e., epidermis) with distinct changes (i.e., hyperkeratosis) to the skin protein keratin. The layer below the epidermis, referred to as the dermis, shows an increase in several inflammatory white blood cell types.
- Blood tests including a complete blood cell count (CBC), a comprehensive metabolic panel (CMP) that includes liver and kidney function tests, and a thyroid hormone panel may be beneficial for diagnosing an underlying systemic disease that may be contributing to the prurigo nodularis.
- Behavioral treatments for prurigo nodularis include ways to prevent scratching and dryness, such as keeping fingernails short, wearing long sleeves, wearing gloves, bandaging lesions, cleaning skin with gentle cleansers, keeping skin moisturized with non-irritating lotions, and avoiding warm environments to reduce sweating. Recommended anti-itch lotions include calamine, menthol, and camphor lotions.
- Moisturizers such as petroleum jelly, fragrance-free and ceramide-rich creams or ointments, and fragrance-free oatmeal or hyaluronic acid creams.
- Second generation oral antihistamines such as Zyrtec, Xyzal, Allegra, Claritin, or Clarinex taken on a regular basis. Many patients need 2 to 3 times the regular daily dose to get adequate relief from the severe itching and/or burning sensation that can be present in some individuals.
- Some patients respond better to first generation sedating antihistamines such as Palgic, Periactin, Atarax, or Benadryl.
- Topical medications such as corticosteroids (e.g., triamcinolone, fluocinonide, betamethasone, mometasone, clobetasol, fluticasone, desoxymetasone), calcineurin inhibitors (e.g., pimecrolimus, tacrolimus), capsaicin (the spicy ingredient in chili peppers), and vitamin D.
- Phototherapy: Exposing affected areas of the skin to specific wavelengths of ultraviolet (UV) light may help reduce the itchiness and inflammation of the skin.
- In 2022, dupilumab (i.e., Dupixent), an interleukin-4 receptor alpha antagonist, was approved by the U.S. Food and Drug Administration (FDA) to treat adults with prurigo nodularis. It is a subcutaneous (SQ) injection which can be self-administered under the skin every 2 weeks.
- In 2024, nemolizumab (i.e., Nemluvio), an interleukin-31 receptor antagonist, was approved by the FDA to treat adults with prurigo nodularis. It is a subcutaneous (SQ) injection administered every 4 weeks.
- Immunosuppressants such as cyclosporin, azathioprine, and methotrexate are reserved for the most resistant cases of prurigo nodularis because they affect more body systems and can have more serious side effects.


 Now that Summer is almost here, people tend to spend a lot of time outdoors. Whether it be going to the beach, swimming at the neighborhood pool, playing baseball or softball, having a picnic, fishing, hiking, riding bicycles, gardening, or any other outside activity, people are more likely to be outdoors now than in any other season of the year. Since the general public is outdoors more in the Summers, it should be noted that there are a lot of outdoor allergens that they are being exposed to when outside.
Now that Summer is almost here, people tend to spend a lot of time outdoors. Whether it be going to the beach, swimming at the neighborhood pool, playing baseball or softball, having a picnic, fishing, hiking, riding bicycles, gardening, or any other outside activity, people are more likely to be outdoors now than in any other season of the year. Since the general public is outdoors more in the Summers, it should be noted that there are a lot of outdoor allergens that they are being exposed to when outside. Histamine is a biogenic amine (i.e., an
Histamine is a biogenic amine (i.e., an  Individuals with pollen allergies may be affected throughout the year, depending on where they live or travel. In the
Individuals with pollen allergies may be affected throughout the year, depending on where they live or travel. In the  Although Primatene Mist became available in 1967, the FDA took it off the market in 2011, as it contained propellants called chlorofluorocarbons (CFC’s) which are harmful to the environment as they deplete ozone from the atmosphere. However, Primatene mist was recently reintroduced into the market with a newer propellant called hydrofluoroalkanes (HFA’s), which are environment friendly. Primatene Mist temporarily opens up the airways in the lungs thus offering a very short-term relief from shortness of breath and/or wheezing. It is approved only for individuals with an established prior diagnosis of asthma. It is used for the temporary relief of mild symptoms of intermittent asthma in patients aged 12 years or older and should not be used as a replacement for prescription asthma medications. Primatene Mist can do more harm than good if used for a chronic cough, for instance, without a known cause.
Although Primatene Mist became available in 1967, the FDA took it off the market in 2011, as it contained propellants called chlorofluorocarbons (CFC’s) which are harmful to the environment as they deplete ozone from the atmosphere. However, Primatene mist was recently reintroduced into the market with a newer propellant called hydrofluoroalkanes (HFA’s), which are environment friendly. Primatene Mist temporarily opens up the airways in the lungs thus offering a very short-term relief from shortness of breath and/or wheezing. It is approved only for individuals with an established prior diagnosis of asthma. It is used for the temporary relief of mild symptoms of intermittent asthma in patients aged 12 years or older and should not be used as a replacement for prescription asthma medications. Primatene Mist can do more harm than good if used for a chronic cough, for instance, without a known cause. Pollen food allergy syndrome (PFAS), also known as oral allergy syndrome, is a condition in which there is first a “sensitization” of the immune system to various pollens and subsequent “reactions” when exposed to these pollens. Secondly, there is a similarity of the protein allergens in the pollen and the protein allergens of certain raw or fresh fruits and/or vegetables. The individual’s immune system, which has been previously sensitized to pollen, will also react to the similarly structured proteins in the raw or fresh fruits and/or vegetables. As a result, when a person who has a pollen allergy (usually trees and/or weeds) eats certain raw or fresh fruits and/or vegetables, that individual’s immune system “thinks” that it is being exposed to pollen proteins when in fact it is being exposed to fruit and/or vegetable proteins that have a very similar chemical structure to the pollen proteins. The body in turn reacts to the fresh fruit and/or vegetable proteins in a similar fashion as a typical allergic reaction but is usually more localized to where the food makes direct contact, such as the lips, tongue, palate, ears, gums, and/or throat. Essentially, there is a cross-reaction to the fresh fruit and/or vegetable because that food is mistaken for pollen and thus reacts in a similar way except the reaction is mostly where contact occurs between the food and the mouth. Note that if the fruit or vegetable is cooked, the pollen food allergy reaction does not usually take place because the heating of the fruit and/or vegetable denatures the protein resulting in the immune system not recognizing this denatured protein anymore because the altered structure of the protein does not look like the pollen protein (allergen) anymore.
Pollen food allergy syndrome (PFAS), also known as oral allergy syndrome, is a condition in which there is first a “sensitization” of the immune system to various pollens and subsequent “reactions” when exposed to these pollens. Secondly, there is a similarity of the protein allergens in the pollen and the protein allergens of certain raw or fresh fruits and/or vegetables. The individual’s immune system, which has been previously sensitized to pollen, will also react to the similarly structured proteins in the raw or fresh fruits and/or vegetables. As a result, when a person who has a pollen allergy (usually trees and/or weeds) eats certain raw or fresh fruits and/or vegetables, that individual’s immune system “thinks” that it is being exposed to pollen proteins when in fact it is being exposed to fruit and/or vegetable proteins that have a very similar chemical structure to the pollen proteins. The body in turn reacts to the fresh fruit and/or vegetable proteins in a similar fashion as a typical allergic reaction but is usually more localized to where the food makes direct contact, such as the lips, tongue, palate, ears, gums, and/or throat. Essentially, there is a cross-reaction to the fresh fruit and/or vegetable because that food is mistaken for pollen and thus reacts in a similar way except the reaction is mostly where contact occurs between the food and the mouth. Note that if the fruit or vegetable is cooked, the pollen food allergy reaction does not usually take place because the heating of the fruit and/or vegetable denatures the protein resulting in the immune system not recognizing this denatured protein anymore because the altered structure of the protein does not look like the pollen protein (allergen) anymore. Spring is here! This means that quite a few Washingtonians will be pretty miserable as they will be suffering from
Spring is here! This means that quite a few Washingtonians will be pretty miserable as they will be suffering from  Food protein-induced enterocolitis syndrome (FPIES) is a rare condition that causes gastrointestinal symptoms several hours after consumption of certain foods by an individual who has an intolerance to that food. The prevalence rate in the United States is approximately 0.5%. The most common types of food allergy in children and adults are mediated by an antibody called IgE. Food allergies may result in adverse reactions which in some cases may be very severe and even life-threatening in some that may occur within minutes of ingestion of the offending food. The IgE antibodies are specific to the food that causes the reaction.
Food protein-induced enterocolitis syndrome (FPIES) is a rare condition that causes gastrointestinal symptoms several hours after consumption of certain foods by an individual who has an intolerance to that food. The prevalence rate in the United States is approximately 0.5%. The most common types of food allergy in children and adults are mediated by an antibody called IgE. Food allergies may result in adverse reactions which in some cases may be very severe and even life-threatening in some that may occur within minutes of ingestion of the offending food. The IgE antibodies are specific to the food that causes the reaction.  Some individuals have episodes of swelling or “angioedema” of various tissues that may occur without any known rhyme or reason. They may have 1 episode or they may have multiple or recurrent episodes. Most people with this condition are very surprised and nervous when they notice an area of their body swelling up right in front of their eyes. The swelling can occur on any part of the body or even internally. They may occur by themselves or they may be accompanied with
Some individuals have episodes of swelling or “angioedema” of various tissues that may occur without any known rhyme or reason. They may have 1 episode or they may have multiple or recurrent episodes. Most people with this condition are very surprised and nervous when they notice an area of their body swelling up right in front of their eyes. The swelling can occur on any part of the body or even internally. They may occur by themselves or they may be accompanied with  Four viral infections are surging in the country this year. Three of them are respiratory viruses and one is a gastrointestinal infection. Influenza (“flu”) usually tends to peak in the Winter. The Centers for Disease Control’s (CDC) statistics reveal that more than 30% of the lab tests were positive for the flu in January of this year and the numbers are climbing. 16 deaths related to influenza were reported, bringing the total to 47 deaths so far this season. Respiratory syncytial virus (RSV) numbers peaked in January of this year and are slowly dropping in case numbers.
Four viral infections are surging in the country this year. Three of them are respiratory viruses and one is a gastrointestinal infection. Influenza (“flu”) usually tends to peak in the Winter. The Centers for Disease Control’s (CDC) statistics reveal that more than 30% of the lab tests were positive for the flu in January of this year and the numbers are climbing. 16 deaths related to influenza were reported, bringing the total to 47 deaths so far this season. Respiratory syncytial virus (RSV) numbers peaked in January of this year and are slowly dropping in case numbers.
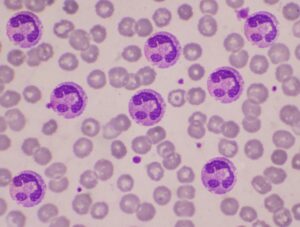 In individuals who are atopic, (i.e., people with a higher incidence of allergic disorders), there will be a higher number of eosinophils in the blood. When there are higher number of eosinophils in the blood than normal, the condition is called eosinophilia. In a disorder named hypereosinophilic syndrome (HES), there are much higher numbers of eosinophils in the blood. Individuals with hypereosinophilic syndrome usually have more than 1,500 eosinophils per microliter in their blood for 6 months or more, and the cause cannot be identified. In addition to being located in the bloodstream, the eosinophils in hypereosinophilic syndrome may also accumulate in various tissues. This excessive eosinophil deposition into the tissues may lead to tissue damage and loss of function.
In individuals who are atopic, (i.e., people with a higher incidence of allergic disorders), there will be a higher number of eosinophils in the blood. When there are higher number of eosinophils in the blood than normal, the condition is called eosinophilia. In a disorder named hypereosinophilic syndrome (HES), there are much higher numbers of eosinophils in the blood. Individuals with hypereosinophilic syndrome usually have more than 1,500 eosinophils per microliter in their blood for 6 months or more, and the cause cannot be identified. In addition to being located in the bloodstream, the eosinophils in hypereosinophilic syndrome may also accumulate in various tissues. This excessive eosinophil deposition into the tissues may lead to tissue damage and loss of function.
 Winter is around the corner and so are the annoying allergy symptoms that some individuals experience during this time of the year. Classically, in the
Winter is around the corner and so are the annoying allergy symptoms that some individuals experience during this time of the year. Classically, in the  Much of the information from the past decade regarding when to introduce peanuts into the diet of infants has been reviewed recently and subsequently revised. Research over the past 9 years shows that early introduction and regular consumption of peanuts decreases the risk of developing a peanut allergy. It is no longer recommended that parents delay the introduction of peanuts in most children, as delay beyond 12 months may actually increase the risk of peanut allergy.
Much of the information from the past decade regarding when to introduce peanuts into the diet of infants has been reviewed recently and subsequently revised. Research over the past 9 years shows that early introduction and regular consumption of peanuts decreases the risk of developing a peanut allergy. It is no longer recommended that parents delay the introduction of peanuts in most children, as delay beyond 12 months may actually increase the risk of peanut allergy.









