December 09, 2019 | Black & Kletz Allergy
 What are some of the causes?
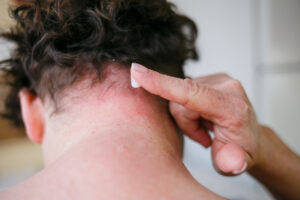
What are some of the causes?
As we enter into the season of colder days and nights in the Washington, DC metropolitan area, we are exposed to colder and drier air. The cold and dry air in conjunction with lower humidity levels predispose individuals to flare-ups of eczematous skin conditions.
Layers of clothing during outdoor activities and returning to overheated homes can trigger a cycle of sweating, itching, scratching, and irritation. Dry heat from our furnaces will evaporate the normal protective oils of one’s skin which may lead to cracking of the skin.
The smoke emitted by indoor fireplaces and wood burning stoves in combination with exposure to dust and dust mites may cause exacerbations of allergies, eczema, and asthma in individuals predisposed to these conditions. Parched air can dry up the normal moisture in the mucus membranes leading to nose bleeds as well as a burning sensation in the eyes.
The pile of wet leaves in people’s yards create a breeding ground for the molds to grow and their spores may trigger allergic rhinitis (i.e., hay fever), asthma, and eczema (i.e., atopic dermatitis) in sensitized individuals. The wool in one’s sweaters can irritate sensitive skin and cause itching (i.e., pruritus) and rashes.
Other common triggers of eczema may include hot water, smoke, sweat, extreme temperatures, perfumes, colognes, cleaning solutions, scented laundry detergent, scented candles, scented soaps, scented shampoos, scented dryer sheets, fabric softeners, pets, molds, pollens, skin infections, stress, and certain foods in people with known food sensitivities.
What can be done in order to improve the situation?
Thorough and regular moisturizing of the skin with emollients (e.g., creams, ointments, lotions, gels) is the best protection against flare- ups of individuals with eczema. Thick oil-based creams and/or ointments generally help protect the skin from excessive dryness better than water-based lotions. “Soak and seal” methods are efficacious in helping prevent the loss of moisture from the skin.
Direct exposures to sources of dry heat (e.g., radiant warmers) should be avoided. If the HVAC system does not have a central humidifier, an ultrasonic water vaporizer in the bedrooms, especially during nights, will reduce excessive dryness of the mucus membranes and the skin.
Long, hot showers can strip the skin of its natural oils. Shorter, lukewarm showers or baths are skin-friendly. Milder soaps, detergents, and shampoos without fragrances are kinder to the skin.
Woolen and synthetic clothes can irritate the skin and cause itching when they are in direct contact with skin. Natural fabrics such as cotton and cashmere are less likely to cause flare-ups of itching and rashes while in direct contact with skin.
In spite of above measures, if eczema does flare-up, one may need to use medications in order to control eczema. Below are a list of several medications used to treat eczema:
1.) In order to manage eczema, it is very common to use topical anti-inflammatory medications (e.g., topical corticosteroids) for a short period of time.
2.) The itching usually responds well to first generation antihistamine medications.
3.) Second generation antihistamines may also help and have the advantage of being generally non-sedating.
4.) Eucrisa (crisaborole) ointment 2% is a nonsteroidal cream that is quite efficacious in the treatment of eczema and has very few side effects. The most common side effect is a mild burning or stinging sensation of the skin where the ointment is applied. Eucrisa ointment 2% is indicated in the treatment of eczema in children ages 2 years of age and older as well as in adults.
5.) Topical immunosuppresants are commonly used in both children and adults. The two most common medications in this class include Protopic (tacrolimus) ointment and Elidel (pimecrolimus) ointment. They are both fairly effective and are steroid-free. Protopic can be used in children 2 years of age and older as well as in adults. Elidel is approved for children 3 months of age and older as well as for adults.
6.) Rarely, a short course of oral corticosteroids may be necessary during severe exacerbations of eczema, although the use of oral corticosteroids is generally avoided due to the potential side effects that corticosteroids can produce.
7.) If all else fails, there is a class of medications called “biologicals” that may be utilized and has been very effective in the treatment of eczema. Dupixent (dupilumab) is currently the only biological that is FDA-approved to treat moderate-to severe-eczema. It is currently approved for adolescents (12 years of age and above) as well as for adults. Of note, Dupixent also is approved for the treatment of asthma in patients 12 years of age and older, as well as in adults with chronic rhinosinusitis with nasal polyps (CRSwNP).
The board certified allergy specialists at Black & Kletz Allergy have expertise in diagnosing and treating eczema as well as other skin conditions [i.e., hives (urticaria), contact dermatitis, poison ivy]. We are board certified to treat both pediatric and adult patients and have been doing so in the Washington, DC, Northern Virginia, and Maryland metropolitan area for more than a half a century. Black & Kletz Allergy has offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All 3 of our offices have on-site parking. For further convenience, our Washington, DC and McLean, VA offices are Metro accessible. Our McLean office location offers a complementary shuttle that runs between our office and the Spring Hill metro station on the silver line. For an appointment, please call our office directly or alternatively, you can click Request an Appointment and we will respond within 24 hours by the next business day. If you suffer from eczema or other skin-related disorder, we are here to help alleviate or hopefully end these unwanted symptoms that have been so bothersome, so that you can enjoy a better quality of life. Black & Kletz Allergy is dedicated to providing the highest quality allergy care in a friendly and professional environment.












