May 24, 2021 | Black & Kletz Allergy
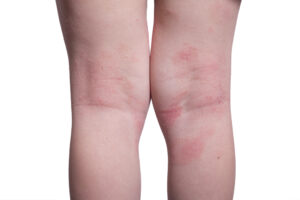
Genetic factors are predominantly implicated in the causation of eczema, but environmental factors such as allergic sensitivity to certain foods and aeroallergens can play a role in aggravating the condition. In most individuals with eczema, the disease follows a remitting and relapsing course throughout one’s life. Exposure to heat, humidity, and other physical factors may also trigger a flare-up of disease activity.
The hallmark of this condition is a disturbance of epidermal-barrier function due to recurrent skin inflammation, which leads to dry skin, pruritis, and IgE-mediated allergen sensitization. Skin lesions may then lead to increased risks of secondary bacterial and/or viral infections.
In addition to generalized dryness of the skin and scattered rashes over the trunk and extremities, incessant itching is usually the most bothersome symptom. It adversely affects the school performance in children and productivity at work in most adults. Uncontrolled atopic dermatitis may also interfere with nighttime sleep and in general, may have a negative impact on one’s quality of life.
Though there is no cure yet for atopic dermatitis, several treatment options are available to control the activity of the disease process and minimize the intensity of symptoms. Traditional management approaches include:
- Emollients – These are moisturizing lotions which hydrate the skin in order to relieve the dryness. They need to be applied all over the body when the skin is still wet after a shower or a bath. They seal the moisture into the skin.
- Topical creams/lotions/ointments – Given in order to reduce inflammation. Corticosteroids are the most common topical anti-inflammatory medications used to reduce the severity of the rash. These agents are available in various strengths and forms. Generally low to medium strength steroids are preferable in order to minimize the side effects such as thinning of the skin and susceptibility to infections. Ointments are preferred to lotions as they can remain on the skin for longer periods. Typically, they are applied twice a day over the affected area for only up to 10 days duration in order to minimize the risks of adverse effects. Ideally, they should not be used over sensitive areas of the body such as the face or groin where they can cause more troublesome side effects such as hypopigmentation. Corticosteroid use in such sensitive areas may also cause higher systemic absorption.
- Non-steroidal topical anti-inflammatory medications – Protopic (i.e., tacrolimus) and Elidel (i.e., pimecrolimus) are non-steroidal topical anti-inflammatory ointments which are alternative medications to topical steroid medications in the treatment of eczema. They can be used long-term but carry a “black box” warning, as some tumors were noted in rodents exposed to these agents.
- Eucrisa – A topical agent approved for the treatment of atopic dermatitis. It is available as a 2% ointment and it can be safely used over the face, as it does not cause steroid-related side effects.
- Dupixent – A biological injectable medication approved for the treatment of uncontrolled asthma as well as atopic dermatitis uncontrolled with topical agents. It works by blocking inflammatory mediators such as IL-4 (i.e., interleukin 4) and IL-13 (i.e., interleukin 13), which contribute to the severity of the disease. The medication is injected under the skin every 2 weeks. The first injection is usually administered in a physician’s offices under close observation and patients are then trained for self-administration of subsequent doses at their homes. Side effects of this Dupixent may include redness and watering of the eyes.
- Antihistamines – Usually utilized for the control of itching in individuals with eczema. First-generation antihistamines [e.g., Benadryl (i.e., diphenhydramine), Atarax (i.e., hydroxyzine)] are generally more effective at relieving the pruritus (i.e., itching) but they are more likely to cause sleepiness. Second-generation antihistamines (e.g., Claritin, Allegra, Zyrtec) are generally not as effective as the first-generation ones for itching but are less sedating and can be dosed once a day.
- Oral corticosteroids – Prednisone, an oral corticosteroid, is occasionally used for short-term bursts to control acute flare-ups of the disease. They are not suitable for long-term use due to the risks of adverse side effects.
Systemic immunosuppressants – Cyclosporine, azathioprine, and methotrexate are immunosuppressants that are rarely used. They are occasionally utilized in order to control severe disease activity; however, their toxicity limits their utility.
As we understand the mechanisms of inflammation in atopic dermatitis in more detail, we are able to target more chemical mediators of disease activity in order to reduce the severity of the symptoms.
Recently, Janus kinase inhibitors or JAK inhibitors have emerged as a novel therapeutic intervention for inflammatory diseases. JAK are intracellular secondary enzyme messengers that transmit extracellular cytokine signaling to the STAT pathway. Inhibition of the JAK-STAT pathway can suppress inflammation and inhibit immune cell activation.
Some of these novel medications which inhibit JAK are currently being used for rheumatological diseases such as rheumatoid arthritis. They are being studied for control of severe atopic dermatitis and clinical trials are revealing very promising results. These JAK inhibitor medications are small molecule agents that are available in both oral [upadacitinib (i.e., Rinvoq), baricitinib (i.e., Olumiant)] and topical [tofacitinib (i.e., Xeljanz)] formulations.
Though none of these medications are yet approved by FDA for the treatment of atopic dermatitis, they remain a promising new therapeutic modality for patients with eczema. They are shown to rapidly and significantly relieve itching as well as reduce the severity of skin lesions.
The board certified allergists at Black & Kletz Allergy have been diagnosing and treating eczema for more than 50 years. We treat both pediatric and adult patients. Black & Kletz Allergy has offices in Washington, DC, McLean, VA (Tysons Corner, VA), and Manassas, VA. All 3 of our locations have on-site parking. For further convenience, our Washington, DC and McLean, VA offices are Metro accessible. Our McLean office location offers a complementary shuttle that runs between our office and the Spring Hill metro station on the silver line. For an appointment, please call our office or alternatively, you can click Request an Appointment and we will respond within 24 hours by the next business day. If you suffer from eczema or other allergic skin conditions, allergies, asthma, or immune disorders, we are here to help alleviate these undesirable symptoms that have been so troublesome, so that you can enjoy a better quality of life. Black & Kletz Allergy is dedicated to providing the highest quality allergy care in a relaxed, caring, and professional environment.












